If you’ve clicked onto this guide, chances are you’re keen to know more about ultrasound-guided injections. Here, we hope to answer all your queries.
What is an ultrasound-guided injection?
Let’s start with the basics…what are they? Well, they’re a remarkable method used by healthcare professionals to deliver medication or therapeutic substances right where they’re needed in your body. How do they do this? They use an ultrasound machine – similar to those used during pregnancy scans – to actually see inside your body in real-time. This way, they can guide the needle to the exact location it needs to be, avoiding crucial structures like nerves and blood vessels.
This technique’s not just impressive; it’s also incredibly versatile. It’s being used for various purposes, such as managing pain, injecting joints, blocking nerves, and even administering specific types of medications or therapies.
And why is it becoming increasingly popular? It’s precision. The accuracy of guided injections not only ensures better results for patients but also significantly reduces the risk of complications. Ultimately, ultrasound-guided injections are revolutionising the way we administer treatments, leading to better patient outcomes.
The science of ultrasound-guided injections – simplified
Interested in the science bit? This section’s for you. (Alternatively, feel free to skip ahead.)
Ultrasound imaging, sometimes called sonography, is like having super-vision that lets healthcare providers (like our physios at W5Physio) see inside your body without making a single cut. It uses high-frequency sound waves to create pictures of what’s happening beneath your skin.
Here’s the magic behind it:
Sound Waves: Ultrasound machines send out high-frequency sound waves. These are too high-pitched for us to hear.
The Transducer: This handheld device is the star of the ultrasound show. It sends out and picks up the sound waves using tiny crystals that can change electrical energy into sound waves, and back again.
Transmission: The transducer is placed on your skin with some gel to help the sound waves travel better. It sends the sound waves into your body.
Reflection: When the sound waves hit different tissues in your body, they bounce back like echoes. The transducer picks up these echoes.
Echo Detection: The transducer changes these echoes back into electrical signals.
Processing: The ultrasound machine’s computer takes these signals, looks at how long the echoes took to come back, and starts building an image.
Image Formation: Using the timing and strength of the echoes, the computer creates a real-time picture of your insides. This can then be seen on a monitor.
Different tissues give off different amounts of echoes, which is why you can see variations in brightness and texture on the ultrasound image.
Ultrasound imaging is safe, painless, and doesn’t involve any radiation. It’s a popular tool for looking at organs, blood vessels, muscles, tendons, and other soft tissues in real-time, helping doctors diagnose and monitor various medical conditions.
And when it comes to injections, ultrasound allows for precise needle guidance, making the procedure safer and more effective.

Why/where are ultrasound-guided injections used?
Ultrasound-guided injections are a versatile tool used in several situations where precise needle placement and accurate medication delivery is key. Examples include:
Joint Pain Relief: They’re often used to inject medications into joints (like the knee, shoulder, hip, or ankle) to manage conditions like arthritis or inflammation.
Tendon Treatment: These injections can be helpful for delivering medication into the sheath of tendons affected by conditions like paratendinitis and tenosynovitis.
Nerve Blocks: Ultrasound guidance can be used to administer nerve blocks for pain management, enabling precise delivery of local anaesthetics or other medications to relieve pain.
Soft Tissue Therapy: They’re used to inject medications into soft tissues, such as muscles or ligaments, to treat conditions like muscle strains, ligament injuries, or fibromyalgia.
Essentially ultrasound-guided injections are a valuable asset across various medical fields, enhancing accuracy and improving patient outcomes. We’ll be sharing some case studies or examples soon. Stay tuned!
Why choose ultrasound-guided injections? (The benefits)
Ultrasound-guided injections use ultrasound imaging to ensure precise placement of injections. Compared to traditional blind injections, they offer several advantages:
Accuracy: Real-time imaging means the needle goes exactly where it needs to, reducing the chances of missing the target or causing unintended damage.
Targeting: Ultrasound helps pinpoint specific areas, like a joint or nerve, especially when these are hard to locate externally. Medication can then be delivered directly to the desired site.
Safety: Real-time imaging helps avoid vital structures like nerves and blood vessels, reducing the risk of accidental injury, especially in complex anatomical areas.
Comfort: By visualising the needle in real-time, healthcare providers can minimise trauma to surrounding tissues, resulting in less pain and discomfort for you.
Outcomes: Accurate needle placement improves treatment effectiveness, leading to better pain relief, improved function, and faster recovery.
Versatility: These injections are used across various medical fields, including orthopaedics, sports medicine, rheumatology, and pain management, and can treat a wide range of conditions.
In a nutshell, ultrasound-guided injections boost accuracy, safety, and effectiveness of treatments, optimising outcomes and improving patient comfort. They’re a valuable tool in the healthcare arsenal.
What to expect during an ultrasound-guided injection procedure
Let’s walk through what you can expect during an ultrasound-guided injection. From pre-procedure prep to the injection itself, here we’ll explain all:
Before the Procedure
Initial Assessment: Your physio will carry out an in-depth assessment of your condition and reason for wanting a guided injection to confirm your suitability for the procedure. Contact us to arrange an assessment/discuss your suitability.
Talk it Out: You’ll have a chat with your physiotherapist about the procedure, its pros and cons, other treatment options, and any special instructions. It’s all about making an informed decision together.
Check-up Time: Your healthcare provider will get the lowdown on your medical history, including any medications you’re taking and any allergies you have.
Food & Drink: Depending on whether sedation or anaesthesia is involved, you might need to fast for a certain period before the procedure.
Dress Code: Go for loose, comfortable clothing that gives easy access to the area being treated.
During the Procedure
Finding the Right Spot: You’ll be positioned so the doctor can easily reach the target area. This could mean lying down, sitting, or standing, depending on the injection site.
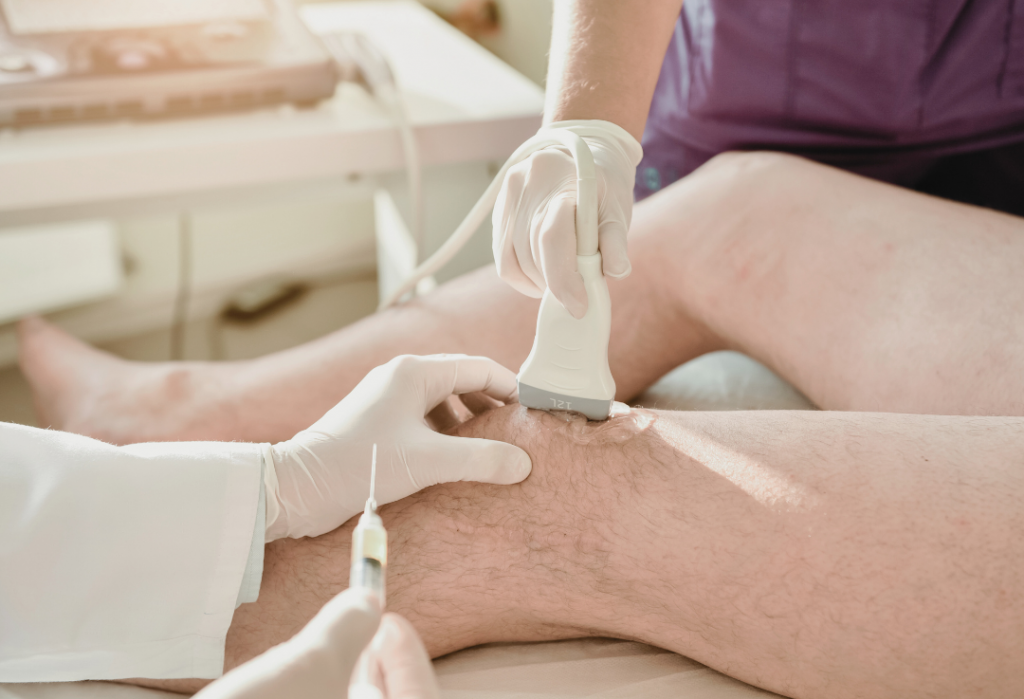
Seeing Inside: The physio will apply a gel to your skin at the injection site. Then they’ll use an ultrasound device, which sends out sound waves, to create real-time images of what’s happening below the surface.
Needle Time: Guided by the ultrasound images, the specialist will insert a thin needle into the right spot. The ultrasound helps make sure the needle placement is spot-on.
Medication Time: Once the needle is in the right place, the medication (like a local anaesthetic or anti-inflammatory drug) will be injected into the target area.
Double-Check: The doctor may use the ultrasound again to confirm that the medication is properly distributed and to check for any immediate changes or improvements.
Remember, everyone’s experience with ultrasound-guided injections will be different. But knowing what to expect can help you feel more prepared and at ease. And of course, if you have any questions or concerns, don’t hesitate to ask us – we’re here to help!
After the Procedure: Post-Procedure Care
Once the injection’s done, here’s what comes next:
Observation: Right after the procedure, you’ll be monitored for about 15-20 minutes to make sure there are no immediate complications or adverse reactions.
Rest and Recovery: Your clinician might recommend taking it easy for a while, depending on the specific injection site and the medication used. This could mean resting at home for at least 2 hours immediately after the procedure, or even limiting certain activities for a few days.
Pain Relief: You might feel some temporary pain relief due to the local anaesthetic. But remember, the full effects of the injected medication may take a bit longer to kick in.
Follow-Up: Your clinician will let you know if you need any follow-up appointments or additional treatments.
Taking Care of the Injection Site
Post-procedure care can also involve looking after the injection site:
Ice, Ice, Baby: It’s common to experience mild soreness at the injection site for 24-48 hours. Ice can help – try applying it for 20 minutes at a time, several times a day.
Pain Management: If you’re still feeling uncomfortable, over-the-counter pain relievers can help.
Take It Easy: You might be able to do some moderate exercise (like leisurely walking or stretching) on the day of the injection but try to avoid heavy lifting for a few days.
Remember, everyone’s recovery process is different. Listen to your body, follow your clinician’s advice, and don’t hesitate to contact us if you have any questions or concerns.
Potential challenges of ultrasound-guided injections
As with any medical procedure, ultrasound-guided injections come with their own set of potential challenges. It’s important to understand these risks and that’s why we ask that you don’t book through our booking page, and instead get in touch with us so we can chat with you about your condition and suitability for the procedure.
Generally, complications from ultrasound-guided injections are generally rare. But there’s always risk of nerve trauma or infection at the injection site. There is also evidence to suggest that long term use of corticosteroid injections used in managing osteoarthritis pain in the hip and knee may potentially lead to further joint damage. And there are links between high doses and frequent use of cortisone shots and incidents of cartilage damage.
Remember, your healthcare provider will always discuss potential risks and benefits with you before proceeding with any treatment. It’s about finding the best solution for your unique health needs.
Final thoughts on guided injections
Ultrasound-guided injections offer a versatile, safe, and accurate way to administer treatments for a wide range of conditions. Their use in ensuring precise needle placement, reducing discomfort, and improving patient outcomes makes them a preferred choice for both healthcare providers and patients.
If you’re dealing with pain or discomfort and traditional treatments haven’t provided the relief you need, it might be time to consider ultrasound-guided injections.
Ready to take the next step? Contact us today to discuss if you feel ultrasound-guided injections could be right for you. Our team of experienced professionals is here to guide you through the process and answer any questions you may have. Don’t let pain hold you back – contact us now to see if ultrasound-guided injections are an option for you.
NB: Ultrasound-guided injections aren’t suitable for everyone, and we’ll carry out an in-depth assessment of every patient before booking you in for the procedure. For this reason, please do not book online. Instead, call 0208 997 1555 to enquire about whether guided injections are a possibility for you.




